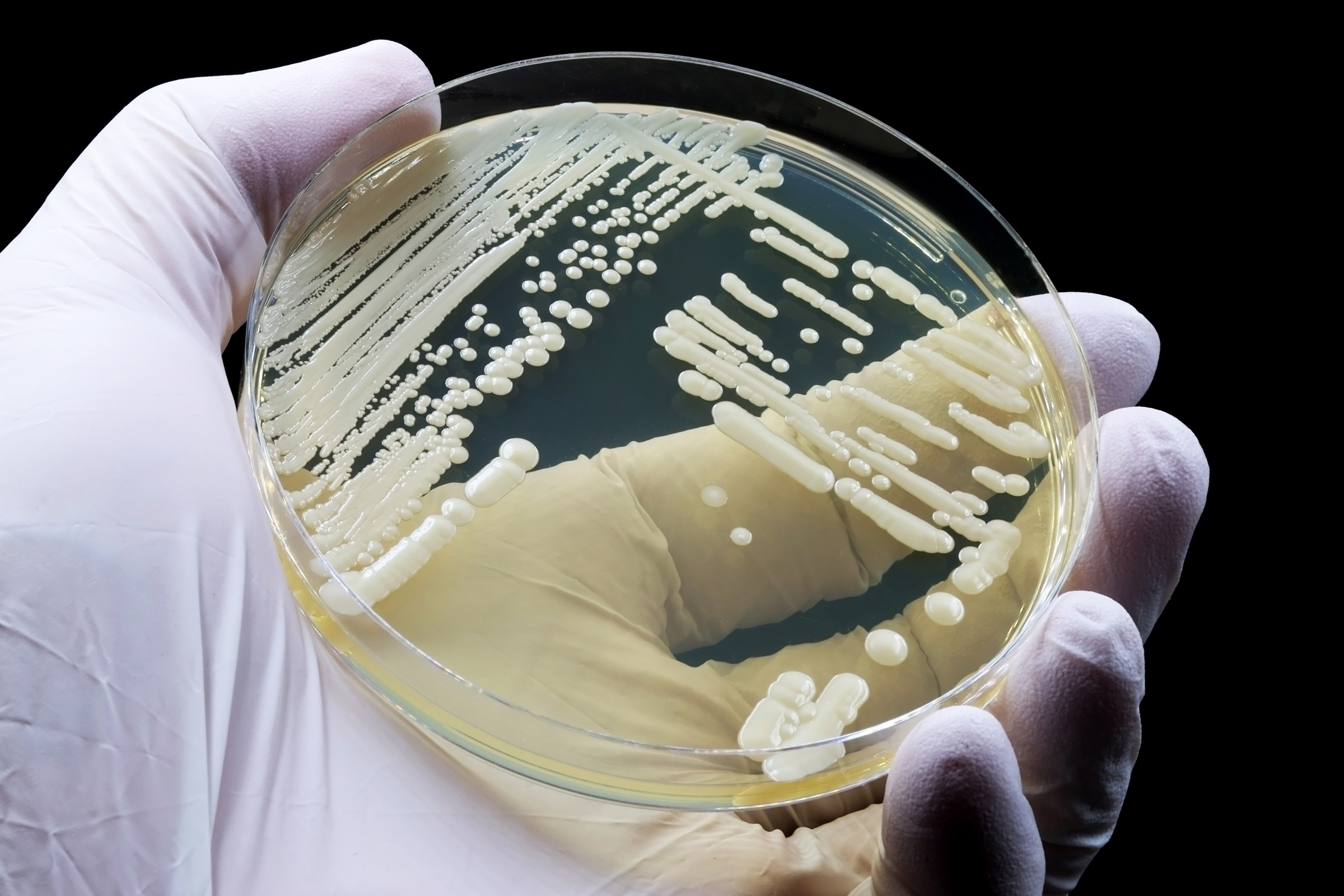
Every day, hospitals’ central sterile processing teams rely on water as they clean and sterilize a variety of medical devices. In this blog, ECRI outlines general considerations to support safe and effective water preparation and use.
Water Quality Categories
There are three categories of water used to process medical devices. The first is utility water. Utility water is suitable for use for point-of-use treatment of a device immediately after patient use, but is not drinking water quality. Utility water is suitable for use for point-of-use treatment of a device immediately after patient use. The temperature of water used for this purpose should not exceed 45C/113F to prevent coagulation of blood and fixation of proteins on the instrument. This water is used for most parts of medical device processing—including flushing, washing, and intermediate rinsing. The notable exception is the final rinse.